Is Stillborn and Stillbirth the Same?
Yes, “stillborn” and “stillbirth” refer to the same phenomenon. Both terms are used to describe the tragic event of a baby being born without signs of life after 20 weeks of pregnancy. A stillborn baby is one who has died in the womb before or during delivery. This heartbreaking occurrence can result from various factors, including complications during pregnancy, congenital abnormalities, or problems during labor and delivery. The terms “stillborn” and “stillbirth” are often used interchangeably in medical and layman’s language to describe the loss of a baby before birth.
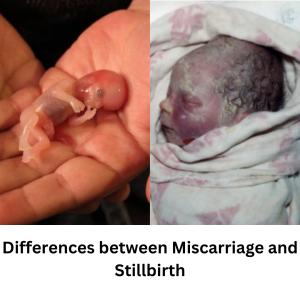
Stillbirth vs. Miscarriage
| Aspect | Stillbirth | Miscarriage |
|---|---|---|
| Definition | Loss of a baby after 20 weeks of gestation or during delivery, with no signs of life. | Loss of a pregnancy before 20 weeks of gestation. |
| Timing | Typically occurs in the later stages of pregnancy, often in the third trimester. | Usually occurs in the first trimester, although it can happen in the early part of the second trimester. |
| Causes | Various factors, including complications with the placenta, umbilical cord issues, infections, and certain medical conditions. | Often due to chromosomal abnormalities, but can also result from maternal health issues, infections, or uterine abnormalities. |
| Emotional Impact | Profound grief due to the loss of a fully developed baby and anticipation of childbirth. | Emotional impact can still be significant, but the physical and emotional connection may be less developed compared to later stages of pregnancy. |
| Medical Attention | Often requires a formal delivery process, and investigations may be conducted to determine the cause. | May involve medical evaluation and monitoring, but the natural process of passing tissue may occur. |